Coronary Artery Disease
Coronary artery disease (CAD) occurs when the coronary arteries that supply blood to the heart muscle become narrowed or blocked due to plaque buildup. This reduces blood flow and oxygen supply to the heart, causing symptoms such as chest pain (angina) and shortness of breath. If untreated, CAD increases the risk of acute coronary syndromes (myocardial infarction), heart failure, arrhythmia, and death (Shahjehan et al., 2024).
Last updated on : 15 Apr, 2026
Read time : 12 mins
Overview of Disease
Coronary artery disease (CAD) is a prevalent cardiovascular condition that affects millions of people worldwide. It is a leading cause of death and disability, making it crucial to understand its causes, symptoms, and treatment options. In this article, we will explore the various aspects of CAD, including its stages, risk factors, and prevention strategies. This will help you to better understand this serious health concern.
What Is Coronary Artery Disease?
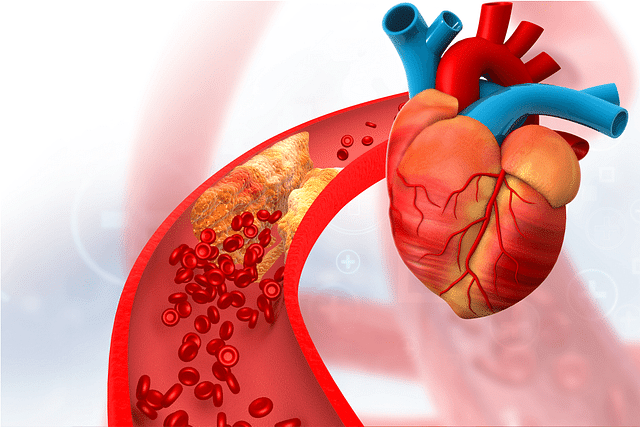
Coronary artery disease, also known as coronary heart disease (CHD) or ischaemic heart disease (IHD), is a condition characterised by the narrowing or blockage of the coronary arteries. These arteries are responsible for supplying oxygen-rich blood to the heart muscle (myocardium). The narrowing or blockage is typically caused by the gradual buildup of plaque, a process called atherosclerosis. Atherosclerosis is an inflammatory, lipid-driven process resulting in plaque formation and vessel remodelling.
The plaque consists of cholesterol, fatty substances, cellular waste products, calcium, and fibrin. As the plaque accumulates, it hardens and narrows the coronary arteries, reducing blood flow to the heart muscle. This reduced blood flow can lead to ischaemia, a condition where the heart muscle receives insufficient oxygen, which may result in chest pain (angina) or myocardial infarction (heart attack).
Key Factors about Coronary Artery Disease
| Category | Details |
| Also Referred as | Coronary Heart Disease (CHD), Ischaemic Heart Disease (IHD), Myocardial Ischaemia |
| Commonly Occurs In | Elderly, Smokers, High Blood Pressure, High Cholesterol, Diabetes, Obesity, Family History |
| Affected Organ | Heart (Coronary Arteries) |
| Type | Stable Coronary Artery Disease (SCAD), Acute Coronary Syndrome (ACS) |
| Common Signs | Chest Pain, Angina, Shortness of Breath, Fatigue, General Weakness |
| Consulting Specialist | Cardiologist |
| Treatment Procedures | Percutaneous Coronary Intervention (PCI), Coronary Artery Bypass Grafting (CABG), Medications (Aspirin, Beta Blockers, Nitroglycerin, Statins) |
| Managed By | Statins, ACE inhibitors, Nitrates, Calcium channel blockers |
| Mimicking Condition | Pulmonary Embolism, Pneumonia, Anxiety Attacks |
Symptoms of Coronary Artery Disease
The symptoms of coronary artery disease can vary from person to person. In the early stages, there may be no noticeable symptoms at all. However, as the disease progresses, you may experience the following:
Chest Pain (angina): This is the most common symptom, often described as a squeezing, pressure, heaviness, tightness, or pain in the chest. The pain may travel to the shoulders, arms, back, or jaw.
Shortness of Breath: You may feel like you can't catch your breath, especially during physical activity.
Fatigue: Unusual tiredness can occur due to the heart not pumping enough blood to meet the body's needs.
Heart Palpitations: You may experience irregular heart rhythms or a fluttering sensation in the chest.
Dizziness: Feeling lightheaded or dizzy can be a result of reduced blood flow to the heart.
It's important to note that in women, the symptoms can be more subtle. Symptoms may include pain in the middle of the back, unexplained shortness of breath, or jaw discomfort. Early recognition of these symptoms is crucial in preventing further complications, such as heart attacks. If you suspect a heart attack, seek emergency medical treatment immediately.
Stages of Coronary Artery Disease
Coronary artery disease progresses through several stages, each with its characteristics and potential complications:
- Early-stage CAD: In the initial stage, plaque begins to accumulate in the coronary arteries. This buildup may not cause any noticeable symptoms, as the arteries are not significantly narrowed. However, this stage marks the beginning of the disease process and highlights the importance of early detection and intervention.
- Chronic CAD: A spectrum of clinical states caused by fixed atherosclerotic narrowing or prior coronary events. Patients may have stable angina symptoms, ischaemic equivalents, or be asymptomatic but at risk. In this stage, individuals may experience symptoms such as mild chest pain (angina) or shortness of breath during physical exertion. These symptoms occur because the narrowed arteries struggle to provide sufficient blood flow to meet the heart's increased oxygen demand during activity.
- Acute CAD: The most critical stage of CAD is acute CAD, which occurs when a plaque ruptures suddenly, causing a blood clot (thrombus) to form. The blood clot can partially or completely block the coronary artery, leading to severe ischaemia or a heart attack. Symptoms of acute CAD include intense chest pain, shortness of breath, sweating, nausea, and dizziness. Prompt medical attention is crucial in this stage to minimise damage to the heart muscle and prevent life-threatening complications (Byrne et al., 2023).
Causes of Coronary Artery Disease
Coronary artery disease occurs when the blood vessels that carry blood to the heart become blocked and narrow. This blockage is typically due to the buildup of plaque, a fatty substance, in the coronary arteries. Over time, the plaque buildup can cause the arteries to narrow and stiffen, restricting blood flow to the heart.
Several factors can contribute to the development of CAD, including:
High blood pressure
High cholesterol
Smoking
Obesity
Diabetes
Understanding these causes can help you identify your risk factors for developing coronary artery disease and take steps to prevent it.
Risk Factors
Several factors can increase your risk of developing coronary artery disease. These include:
High blood pressure
High blood cholesterol levels
Tobacco smoking
Diabetes
Obesity
Physical inactivity
Unhealthy eating habits
Emotional stress
Family history of CAD
Age: Men are at higher risk after 45 years old, while women are at higher risk after 55 years old
By understanding these risk factors, you can take steps to reduce your chances of developing CAD. Also, you can manage the disease if you have already been diagnosed.
Complications
Coronary artery disease can lead to several serious and potentially life-threatening complications if left untreated. Some of the most common complications include:
- Heart Attack: When a coronary artery becomes completely or partially blocked, it can cause damage to the heart muscle. This can result in a heart attack.
- Heart Failure: Over time, CAD can weaken the heart muscle. This makes it difficult for the heart to pump enough blood to meet the body's needs, leading to heart failure.
- Arrhythmias: CAD can cause irregular heartbeats, which can lead to further complications such as ventricular tachycardia and sudden cardiac death (Shahjehan et al., 2024).
- Angina: Reduced blood flow to the heart muscle due to CAD can cause chest pain or discomfort, known as angina.
- Stroke: The risk factors for CAD also increase the risk of stroke. This occurs when the arteries supplying blood to the brain are narrowed or blocked.
- Peripheral Artery Disease: CAD can lead to narrowed arteries in the legs, causing leg pain during exercise.
- Sudden Cardiac Arrest: A severe complication of CAD that can result in sudden cardiac death if not treated promptly.
- Aneurysm: Atherosclerosis associated with CAD may contribute to aneurysm formation in arterial walls, although this is less directly linked.
Preventing these complications is crucial, and adopting a healthy lifestyle can significantly reduce the risk of developing CAD and its associated complications.
Prevention of Coronary Artery Disease
Preventing CAD involves making lifestyle changes and adopting healthy habits. Some key steps to prevent CAD include:
Quit Smoking: Smoking is a major risk factor for CAD, so quitting can significantly reduce your risk.
Eat a Healthy Diet: Consume a low-sodium diet rich in fruits, vegetables, and whole grains to promote heart health.
Maintain a Healthy Weight: Manage your weight through a balanced diet and regular exercise to reduce the risk of CAD.
Exercise Regularly: Engage in regular physical activity to maintain cardiovascular health and reduce the risk of CAD.
Manage Stress: Practice stress-reducing techniques such as yoga or meditation to help control blood pressure and reduce the risk of CAD.
In addition to these lifestyle changes, it's important to work with your doctor to manage any underlying health conditions. This includes managing conditions like high blood pressure, high cholesterol, or diabetes.
Diagnosis & Tests
Diagnosing CAD typically involves a combination of physical examination, medical history, and various tests. Your doctor will perform a physical examination to assess your overall health and listen for abnormal heart sounds. They will also ask about your medical history and family history to identify any potential risk factors for CAD.
Some common tests used to diagnose CAD include:
- Electrocardiogram (ECG): This test records the electrical activity of your heart and can help detect any abnormalities in heart rhythm (Shahjehan et al., 2024).
- Stress Test: During a stress test, you will be asked to exercise on a treadmill or stationary bike while your heart rate, blood pressure, and ECG are monitored. This test can help detect any changes in heart function during physical activity.
- Echocardiogram: This test uses sound waves to create images of your heart, allowing your doctor to assess its structure and function.
- Coronary Angiogram: In this test, a special dye is injected into your coronary arteries. Then, X-ray images are taken to detect any blockages or narrowing of the arteries.
- Cardiac CT Scan or MRI: These imaging tests can provide detailed images of your heart and coronary arteries. This helps to identify any blockages or other abnormalities.
Non-invasive risk stratification may include coronary artery calcium scoring, CT coronary angiography, or functional stress testing, depending on pre-test probability and available resources.
Early diagnosis and management of CAD are essential for preventing complications and improving health outcomes. If you experience symptoms such as chest pain or shortness of breath, seek medical attention promptly.
Treatment & Management
Medications play a crucial role in managing coronary artery disease (CAD) by controlling risk factors, alleviating symptoms, and preventing complications. Commonly prescribed medications include:
1. Blood Pressure Control
- Beta-blockers: Medications like metoprolol, propranolol, atenolol, and sotalol lower heart rate and reduce blood pressure, decreasing the heart’s workload.
- Angiotensin-Converting Enzyme (ACE) Inhibitors: Medicines such as ramipril and lisinopril help relax blood vessels, lower blood pressure, and protect heart function.
- Angiotensin II Receptor Blockers (ARBs): Alternatives for those intolerant to ACE inhibitors, including telmisartan, losartan, and valsartan, which also help control blood pressure.
- Calcium Channel Blockers: Medications like verapamil, diltiazem, amlodipine, and nifedipine relax blood vessels, improving blood flow and reducing blood pressure.
2. Cholesterol Management
- Statins (HMG-CoA Reductase Inhibitors): Medicines such as rosuvastatin, atorvastatin, lovastatin, and simvastatin lower LDL cholesterol, reducing plaque buildup in arteries.
3. Angina (Chest Pain) Relief
- Nitrates: Nitroglycerin helps relax blood vessels and improve blood flow to the heart, relieving angina symptoms.
- Calcium Channel Blockers: Amlodipine, verapamil, diltiazem, and nifedipine also help in angina management by improving blood circulation.
4. Prevention of Blood Clots
- Platelet Inhibitors: Aspirin and clopidogrel prevent blood clot formation, reducing the risk of heart attacks.
5. Treatment Considerations
- The choice of medication depends on individual patient needs, underlying conditions, and response to treatment.
- Regular medical follow-ups are essential to monitor effectiveness and manage potential side effects.
- A combination of medications may be prescribed to optimise heart health and prevent disease progression.
In patients with prior PCI or ACS, dual antiplatelet therapy duration is guided by clinical context; lipid-lowering and blood pressure goals should be aggressively managed as per guidelines (Lawton et al., 2022).
When to See a Doctor?
Be aware of the signs and symptoms of CAD and seek medical attention if you experience concerning symptoms. If chest pain suggestive of myocardial ischaemia occurs (central chest pressure, sweating, syncope, severe breathlessness), seek emergency medical care immediately (Byrne et al., 2023). These symptoms may indicate a worsening of your condition or the development of complications.
Even if you are not experiencing symptoms, regular check-ups with your doctor are essential for monitoring CAD and adjusting your management plan as needed. Your doctor may perform tests such as ECGs, stress tests, or coronary angiograms to assess disease severity and guide treatment decisions.
By working closely with your doctor and attending regular follow-ups, you can effectively manage CAD and reduce the risk of complications.
Key Takeaways
Coronary artery disease is managed through a comprehensive approach that includes lifestyle changes, medications, and possible surgical interventions.
Adopting a healthy lifestyle, which involves quitting smoking, eating a balanced diet, exercising regularly, maintaining a healthy weight, and managing stress, is crucial for managing CAD.
Medications such as statins, beta-blockers, ACE inhibitors, and aspirin play a vital role in preventing further cardiovascular events and managing symptoms.
Early diagnosis and regular check-ups with your doctor are important for optimal management of CAD and reducing cardiovascular risks. If you experience symptoms like chest pain, shortness of breath, or excessive fatigue, seek medical attention promptly.
FAQs
What steps can be taken to reduce blockage in coronary arteries?
Regular exercise, a healthy diet, quitting smoking, maintaining a healthy weight, managing stress, and taking prescribed medications can help reduce coronary artery blockages.
Is it possible to reduce the severity of coronary artery disease?
Yes, coronary artery disease can be reduced through lifestyle modifications such as dietary changes, regular physical activity, smoking cessation, and managing cholesterol and blood pressure levels.
Are there any drinks that can help cleanse the arteries?
While no single drink can directly clean arteries, consuming antioxidant-rich beverages like green tea, pomegranate juice, and cranberry juice may support cardiovascular health.
How can calcium deposits in arteries be removed naturally?
There is no natural method to directly remove existing calcium deposits from arteries. However, adopting a healthy lifestyle can slow the progression of calcification.
Can eating bananas help clear blocked arteries?
Bananas alone cannot clear blocked arteries. However, they are part of a balanced diet that promotes overall cardiovascular health due to their potassium content.
Is it possible to remove heart blockages without undergoing surgery?
In some cases, lifestyle changes, medications, and non-surgical procedures like angioplasty and stenting can help manage and reduce heart blockages without the need for surgery.
Which fruits are beneficial for maintaining healthy arteries?
Fruits rich in antioxidants, such as berries, citrus fruits, and pomegranates, may help protect the arteries from damage and support cardiovascular health.
Do tomatoes have a positive effect on arterial health?
Yes, tomatoes are a good source of lycopene. It's an antioxidant that may help reduce inflammation and oxidative stress in the arteries, promoting their health.
References
- Byrne, R. A., Rossello, X., Coughlan, J. J., Barbato, E., Berry, C., Chieffo, A., Claeys, M. J., Dan, G.-A., Dweck, M. R., Galbraith, M., Gilard, M., Hinterbuchner, L., Jankowska, E. A., Jüni, P., Kimura, T., Vijay Kunadian, Leosdottir, M., Lorusso, R., Roberto F.E. Pedretti, & Rigopoulos, A. (2023). 2023 ESC Guidelines for the management of acute coronary syndromes. European Heart Journal, 44(38). https://doi.org/10.1093/eurheartj/ehad191
- Bansal, A., & Hiwale, K. (2023). Updates in the Management of Coronary Artery Disease: A Review Article. Cureus, 15(12). https://doi.org/10.7759/cureus.50644
- Shahjehan, R. D., Bhutta, B. S., & Sharma, S. (2024). Coronary artery disease. National Library of Medicine; StatPearls Publishing. https://www.ncbi.nlm.nih.gov/books/NBK564304/
- Virani, S. S., Newby, L. K., Arnold, S. V., Bittner, V., Brewer, L. C., Demeter, S. H., Dixon, D. L., Fearon, W. F., Hess, B., Johnson, H. M., Kazi, D. S., Kolte, D., Kumbhani, D. J., LoFaso, J., Mahtta, D., Mark, D. B., Minissian, M., Navar, A. M., Patel, A. R., & Piano, M. R. (2023). 2023 AHA/ACC/ACCP/ASPC/NLA/PCNA Guideline for the Management of Patients with Chronic Coronary disease: A Report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines. Circulation, 148(9). https://doi.org/10.1161/CIR.0000000000001168
- Lawton, J. S., Tamis-Holland, J. E., Bangalore, S., Bates, E. R., Beckie, T. M., Bischoff, J. M., Bittl, J. A., Cohen, M. G., DiMaio, J. M., Don, C. W., Fremes, S. E., Gaudino, M. F., Goldberger, Z. D., Grant, M. C., Jaswal, J. B., Kurlansky, P. A., Mehran, R., Metkus, T. S., Nnacheta, L. C., & Rao, S. V. (2022). 2021 ACC/AHA/SCAI Guideline for Coronary Artery Revascularization: a Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation, 145(3). https://doi.org/10.1161/cir.0000000000001038
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesHealth LibraryDiseases & Health ConditionsAyurvedaUnderstanding Generic MedicinesAll MedicinesAll BrandsNeed HelpFAQSecuritySavings CalculatorSubscribe
Registered Office Address
Grievance Officer
Download Truemeds
Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v4.25.2
2026 - Truemeds | All rights reserved. Our content is for informational purposes only. See additional information.
Our Payment Partners










































