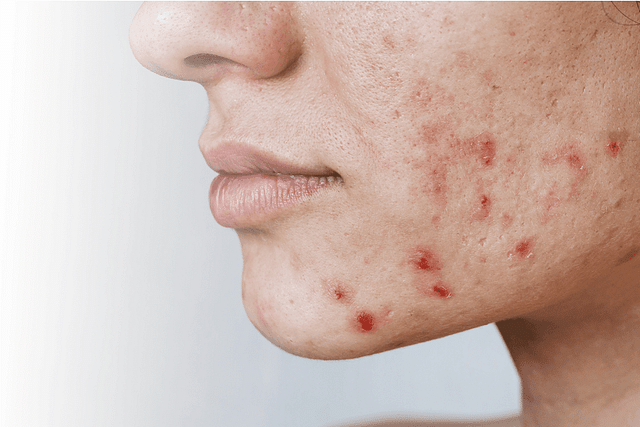
Acne
Acne is a common skin condition that occurs when hair follicles become clogged with oil and dead skin cells, leading to the formation of pimples, blackheads, and whiteheads. It affects people of all ages but is most prevalent during puberty. Acne can be classified into four grades based on severity and includes various types such as comedonal, inflammatory, and nodulocystic acne.
Last updated on : 09 Dec, 2024
Read time : 14 mins
Overview of Disease
Acne is a prevalent skin disorder that affects millions of people worldwide. It is characterised by the appearance of various types of lesions on the skin, particularly in areas with a high density of oil glands, such as the face, back, and chest. While acne is most common among teenagers, it can also affect adults, especially women. Understanding the causes, stages, and types of acne is crucial for effective management and treatment of this condition.
What is Acne?
Acne is a multifactorial skin condition that results from a combination of excess sebum production, dead skin cell accumulation, bacterial growth, and inflammation within hair follicles. Sebaceous glands, which are connected to hair follicles, produce an oily substance called sebum. When the follicles become clogged with a mixture of sebum and dead skin cells, it creates an ideal environment for the proliferation of bacteria, particularly Propionibacterium acnes. This process leads to the development of various types of acne lesions, ranging from mild to severe.
Key Factors about Acne
| Category | Details |
| Also Referred as | Acne vulgaris |
| Commonly Occurs In | Teenagers, though it affects people of all ages |
| Affected Organ | Skin, particularly areas with high oil gland concentration (face, forehead, chest, upper back, shoulders) |
| Type | Comedonal, papular, pustular, nodular, cystic (or nodulocystic) |
| Common Signs | Whiteheads, blackheads, papules, pustules, nodules, cysts |
| Consulting Specialist | Dermatologist |
| Treatement Procedures | Topical and oral medications (e.g., benzoyl peroxide, antibiotics, retinoids), lifestyle changes, minor procedures |
| Managed By | Retinoids (Retinoic acid, Tretinoin & Adapalene), Antimicrobials (Azelaic acid), Topical antibiotics (Clindamycin & Azithromycin), Anti-acne agents (Salicylic acid), Systemic antibiotics (Doxycycline & Minocycline), Oral |
| Mimiciking Condition | Folliculitis, rosacea, hidradenitis suppurativa, miliaria |
Types of Acne
Acne can be broadly categorised into three main types based on the predominant lesions present. These include:
Comedonal acne: This type is characterised by the presence of non-inflammatory lesions called comedones.
Whiteheads: These are plugged hair follicles that remain beneath the skin surface, creating small, white or flesh-coloured bumps.
Blackheads: When plugged follicles open up and reach the skin surface, the exposed sebum undergoes oxidation, resulting in a dark appearance.
Inflammatory acne: This type features red, inflamed lesions that occur when bacteria infect the clogged hair follicles.
Papules: These are small, pink, or red bumps that can be tender to the touch and are often surrounded by inflamed skin.
Pustules: Similar to papules, pustules are inflamed bumps that contain visible pus at their tips and are commonly referred to as "pimples."
Nodulocystic acne: This severe form of acne is characterised by large, deep, and painful lesions that extend into deeper layers of the skin.
Nodules: These are solid, large, and painful bumps that form deep within the skin and can persist for weeks or even months.
Cysts: Cysts are pus-filled, painful lesions that can cause significant damage to the skin and often lead to scarring.
Identifying the predominant type of acne lesions is crucial for determining the most suitable treatment approach and minimising the risk of long-term complications such as scarring and hyperpigmentation.
Symptoms of Acne
Acne is a common skin condition characterised by various symptoms that can vary in severity. Key symptoms include:
Comedones: These are non-inflammatory lesions, including open comedones (blackheads) and closed comedones (whiteheads), which form when hair follicles become clogged with oil and dead skin cells.
Papules: Small, red, inflamed bumps that can be tender to the touch. Papules are a sign of inflammation in the hair follicles.
Pustules: Similar to papules but filled with pus, pustules appear as red bumps with a white or yellow centre. They indicate a more advanced inflammatory response.
Nodules: Larger, painful lumps that develop beneath the skin's surface. Nodules are solid and can be quite tender, often requiring more intensive treatment.
Cysts: Deep, painful, pus-filled lesions that can lead to scarring. Cysts are a severe form of acne and are often larger than nodules.
Scarring: Acne can lead to permanent scars, which may appear as depressions or raised areas on the skin after the lesions heal.
Skin changes: The affected areas may appear oily and have an uneven texture, and individuals may experience redness or inflammation around the acne lesions.
Stages of Acne
Acne can be classified into four grades based on the severity and extent of the lesions. The stages of acne include:
Grade 1 (mild acne): This stage is characterised by the presence of a few whiteheads and blackheads, with occasional small, inflamed bumps called papules.
Grade 2 (moderate acne): In this stage, there is an increased number of comedones (whiteheads and blackheads) and a greater frequency of inflammatory papules and pustules.
Grade 3 (severe acne): This stage features numerous comedones, papules, and pustules, as well as the appearance of larger, more painful lesions called nodules.
Grade 4 (cystic acne): The most severe form of acne, this stage is characterised by widespread, large, and painful cysts and nodules that can lead to significant scarring if left untreated.
Causes of Acne
Acne is primarily caused by a combination of factors that lead to the blockage of hair follicles and the overproduction of oil. Some of the causes include:
Hormonal changes: Fluctuations in hormones, particularly during puberty, menstruation, or pregnancy, can increase oil production in the skin, contributing to acne development.
Excess oil production: Overactive sebaceous (oil) glands can lead to excessive sebum production, which can clog pores and create an environment conducive to acne.
Clogged hair follicles: Dead skin cells can accumulate and mix with oil, blocking hair follicles. This can lead to the formation of comedones (blackheads and whiteheads).
Bacteria: The presence of Propionibacterium acnes (P. acnes), a type of bacteria that normally lives on the skin, can contribute to inflammation and infection when follicles are clogged.
Inflammation: The body's immune response to bacteria and clogged follicles can cause inflammation, leading to the red, swollen lesions characteristic of acne.
Diet: Certain dietary factors, such as high glycaemic foods and dairy products, may exacerbate acne in some individuals
Stress: Increased stress levels can trigger hormonal changes that may worsen acne, leading to flare-ups.
Medications: Some medications, such as corticosteroids or certain hormonal treatments, can contribute to acne development.
Genetics: A family history of acne can increase the likelihood of developing the condition, suggesting a genetic predisposition.
Risk Factors
Several factors can increase an individual's likelihood of developing acne, including:
Hormonal changes during puberty, menstruation, pregnancy, and menopause
Genetic predisposition
Certain medications containing corticosteroids, testosterone, or lithium
Diets high in refined carbohydrates, dairy products, or foods with a high glycemic index
Stress
Friction or pressure on the skin from items like helmets, tight collars, or backpacks
Harsh skin care products or excessive face washing
Who's at Risk?
Acne can affect individuals of all ages, but some groups are more susceptible, including:
Adolescents and young adults
Women who experience hormonal fluctuations, such as during menstrual cycles or pregnancy
Individuals with a family history of acne
People with oily skin types
Those who use certain medications that can trigger acne as a side effect
Individuals who consume diets high in refined carbohydrates, dairy, or high-glycemic foods
People who experience high levels of stress
Those who frequently wear items that cause friction or pressure on the skin
Complications
While acne is primarily a skin condition, it can lead to several complications, particularly if not managed properly. These complications include:
Scarring: Acne can cause both atrophic (depressed) and hypertrophic (raised) scars. These scars can be permanent and may require treatments like laser therapy or dermal fillers to improve appearance.
Hyperpigmentation: After acne lesions heal, they can leave behind dark spots or areas of discolouration on the skin, known as post-inflammatory hyperpigmentation. This can take time to fade and may require treatments like chemical peels or topical lightening agents.
Psychological impact: Acne can significantly affect mental health, leading to issues such as low self-esteem, anxiety, and depression. The visible nature of acne can cause distress and social withdrawal for some individuals.
Infection: Infected acne lesions can lead to more severe conditions, such as abscesses, which may require medical intervention or drainage.
Acne fulminans: A rare but severe form of acne that can occur suddenly, causing extensive inflammation, painful nodules, and systemic symptoms like fever. This condition requires immediate medical attention.
Chronic skin changes: Persistent acne can lead to lasting changes in skin texture and appearance, affecting overall skin health.
Prevention of Acne
Preventing acne involves a combination of lifestyle choices and skincare practices. Here are key strategies to help reduce the risk of developing acne:
Maintain a clean skin routine: Gently wash the face twice daily with a mild cleanser to remove excess oil, dirt, and impurities. Avoid harsh scrubs that can irritate the skin.
Moisturise: Use non-comedogenic moisturisers to keep the skin hydrated without clogging pores. Even oily skin needs moisture to maintain balance.
Choose non-comedogenic products: Select makeup, skincare, and haircare products labelled as non-comedogenic, meaning they are less likely to clog pores.
Avoid touching the face: Minimise touching the face, as oils and bacteria from the hands can contribute to clogged pores and irritation.
Manage hair products: Keep hair clean and avoid heavy hair products that can transfer to the skin and clog pores, especially along the hairline.
Healthy diet: Incorporate a balanced diet rich in fruits, vegetables, whole grains, and lean proteins. Some individuals may benefit from reducing high-glycaemic foods and dairy.
Stay hydrated: Drink plenty of water to maintain skin hydration and support overall health.
Sun protection: Use non-comedogenic sunscreen to protect the skin from UV damage, which can exacerbate acne and lead to scarring.
Stress management: Engage in stress-reducing activities such as exercise, meditation, or hobbies, as stress can trigger hormonal changes that worsen acne.
By adopting these preventive measures, individuals can reduce their risk of developing acne and maintain healthier skin.
Diagnosis & Tests
Diagnosing acne typically involves a thorough clinical evaluation by a doctor. The process includes:
Medical history: The doctor will ask about the patient's medical history, including any previous skin conditions, family history of acne, and current medications or skincare products.
Physical examination: A detailed examination of the skin is conducted to assess the type and severity of acne lesions, including the presence of comedones, papules, pustules, nodules, or cysts.
Assessment of symptoms: The provider may enquire about the frequency and duration of breakouts, any associated symptoms (such as pain or itching), and the impact of acne on the patient’s quality of life.
Differential diagnosis: The doctor may rule out other skin conditions that can mimic acne, such as rosacea, folliculitis, or hidradenitis suppurativa, to ensure an accurate diagnosis.
Laboratory tests: In certain cases, blood tests or hormonal evaluations may be recommended to identify underlying hormonal imbalances, especially in adult women with persistent or severe acne.
Treatment & Management
The treatment of acne varies based on its severity and type, typically including a combination of lifestyle changes, topical treatments, and, in some cases, oral medications. Some of the treatment options include:
Topical treatments: Topical treatments often begin with benzoyl peroxide, which is an antibacterial agent that helps reduce inflammation and kill acne-causing bacteria. Salicylic acid aids in unclogging pores and exfoliating the skin. Retinoids help prevent clogged pores and promote cell turnover. Topical antibiotics like clindamycin are also commonly used to reduce bacteria and inflammation on the skin.
Oral medications: For more severe cases, oral medications may be necessary. Oral antibiotics are prescribed for moderate to severe acne to reduce bacteria and inflammation. Hormonal treatments, including birth control pills, can be effective for females by helping to regulate hormones that trigger acne.
Chemical peels: Chemical peels, performed by dermatologists, involve applying a solution to exfoliate the top layer of skin. This treatment can improve acne and reduce scarring by removing dead skin cells and promoting new cell growth.
Laser and light therapies: Laser and light therapies are used to target acne bacteria and reduce inflammation through various light technologies. These treatments may be used in conjunction with other therapies.
Lifestyle and skincare adjustments: Lifestyle and skincare adjustments are crucial for successful treatment. Adopting a gentle skincare routine, using non-comedogenic products, and maintaining a healthy diet can support overall acne management.
Medication for Acne
There are various medications available for treating acne, including:
For mild to moderate acne, topical treatments are commonly used. Benzoyl peroxide is effective in reducing bacteria and inflammation. Salicylic acid helps unclog pores and exfoliate the skin, while retinoids, such as tretinoin, promote cell turnover and prevent new comedones from forming.
Topical antibiotics like clindamycin can also reduce bacteria and inflammation, helping to clear existing lesions.
In cases of moderate to severe acne, oral medications may be necessary. Oral antibiotics, such as doxycycline or minocycline, help decrease bacteria and inflammation from within.
For females, hormonal treatments, including birth control pills and anti-androgens like spironolactone, can regulate hormones that contribute to acne.
Isotretinoin, a powerful oral retinoid, is typically reserved for severe, treatment-resistant cases. It significantly reduces oil production and can lead to long-term remission.
In many instances, a combination of topical and oral medications is utilised to maximise effectiveness. This approach allows for targeted treatment of acne while addressing different contributing factors.
When to See a Doctor?
If you find that your acne is severe, persists for a long time, or significantly impacts your self-esteem and confidence, it's essential to consult with a doctor. Additionally, seek medical advice if over-the-counter acne products do not improve your skin after several weeks of use. If you notice signs of infection, such as increased redness, swelling, warmth, or discharge, it is advisable to see a doctor promptly.
Key Takeaways
Acne is a common skin condition that affects people of all ages, but it is most prevalent in teenagers and young adults.
Various factors, including hormonal changes, genetics, skincare habits, and lifestyle choices, can contribute to the development of acne.
Treatment options for acne include over-the-counter medications, prescription topical and oral treatments, and in-office procedures.
Maintaining a consistent skincare routine, using non-comedogenic products, and adopting a balanced diet and lifestyle can help manage acne and reduce the risk of future breakouts.
If acne is severe, persistent, or causing significant distress, it is important to consult a dermatologist or doctor for personalised advice and treatment options.
FAQs
Is acne considered a disease or a skin condition?
Acne is generally classified as a common skin condition rather than a disease. It involves inflammation of the skin due to clogged hair follicles.
How to remove a pimple overnight?
Removing a pimple overnight is usually not feasible and may worsen inflammation and scarring. Warm compresses and over-the-counter treatments can help reduce its appearance.
Which treatment is best for acne?
The optimal acne treatment depends on the severity. Mild cases may improve with over-the-counter products, while moderate to severe acne often requires prescription medications.
Is vitamin C good for acne?
Although vitamin C has a limited direct impact on acne, it can reduce inflammation and promote skin health. A balanced diet with vitamin C-rich foods supports overall skin well-being.
What are the home remedies for acne / pimples?
While home remedies shouldn't replace medical treatment, maintaining good hygiene, avoiding heavy makeup, eating a balanced diet, staying hydrated, and managing stress may help reduce acne risk.
Can acne be cured with ayurveda?
Ayurvedic treatments may help manage acne symptoms, but they should be used in conjunction with conventional medical treatments for the best results. Consult a qualified Ayurvedic practitioner for personalised advice.
How do I remove my pimple marks?
Pimple marks can be reduced through consistent use of sunscreen, gentle exfoliation, and topical treatments containing ingredients like retinoids, vitamin C, or niacinamide. Consult a dermatologist for stubborn marks.
References
- National Institute of Arthritis and Musculoskeletal and Skin Diseases. (2020). What is acne? Definition & types. https://www.niams.nih.gov/health-topics/acne
- Penn Medicine. (n.d.). Acne - Symptoms and causes. https://www.pennmedicine.org/for-patients-and-visitors/patient-information/conditions-treated-a-to-z/acne
- Yale Medicine. (n.d.). Acne (Acne Vulgaris). https://www.yalemedicine.org/conditions/acne
- Johns Hopkins Medicine. (n.d.). Acne. https://www.hopkinsmedicine.org/health/conditions-and-diseases/acne
- NHS. (n.d.). Acne. https://www.nhs.uk/conditions/acne/
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
...View more
Top-OTC medicines:
...View more
Subscribe
Registered Office Address
Grievance Officer
Download Truemeds

Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v3.7.5
Our Payment Partners