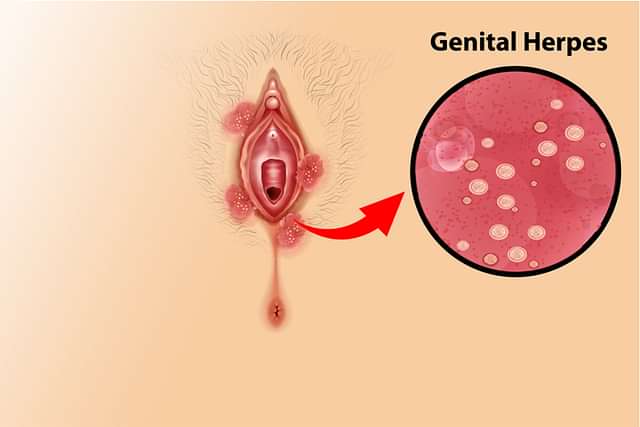
Genital Herpes
Genital herpes is a common sexually transmitted infection (STI) caused by the herpes simplex virus (HSV). It can cause painful blisters or sores on and around the genitals, rectum, and mouth. It is spread through skin-to-skin contact with an infected person. Two main types of HSV cause genital herpes: HSV-1 and HSV-2.
Last updated on : 05 Mar, 2025
Read time : 13 mins
Overview of Disease
Genital herpes is a widespread sexually transmitted infection caused by the herpes simplex virus (HSV). This condition leads to the formation of painful sores or blisters in the genital region. Although there is no permanent cure, being informed about its symptoms and treatment options can help individuals manage outbreaks and reduce transmission risks effectively.
What is Genital Herpes?
Genital herpes is an STI caused by the HSV. This virus can cause painful blisters or sores on and around the genitals, rectum, and mouth. Genital herpes is transmitted through skin-to-skin contact with an infected person, even if they do not have visible symptoms. It is important to note that genital herpes can be transmitted even when no visible sores are present. The HSV virus can be shed from the skin without causing symptoms.
Key Factors about Genital Herpes
| Category | Details |
| Also Referred as | Genital herpes simplex virus (HSV) infection, HSV-2 infection |
| Commonly Occurs In | Adults with multiple sexual partners, women, people with a history of STIs, older people, Black people in the US, men who have sex with men |
| Affected Organ | Genitals, rectum, buttocks, thighs, mouth, anus, urethra, cervix, internal organs (rare) |
| Type | HSV-1, HSV-2 |
| Common Signs | Painful blisters or sores near genitals, anus, or mouth; itching or burning on the skin; flu-like symptoms during the first outbreak; painful urination |
| Consulting Specialist | Primary care physician, gynaecologist, urologist, dermatologist |
| Treatement Procedures | Antiviral medications to manage symptoms and prevent recurrences; comfort measures to alleviate pain and discomfort |
| Managed By | Antiviral medications (acyclovir, valacyclovir, and famciclovir) |
| Mimiciking Condition | Other STIs, skin conditions, or infections causing similar symptoms (e.g., syphilis) |
Types of Genital Herpes
There are two primary types of genital herpes, each caused by a distinct strain of the herpes simplex virus:
HSV-1: This type of HSV is usually responsible for oral herpes, causing cold sores or fever blisters around the mouth. However, it can also cause genital herpes in some cases, particularly through oral-genital contact.
HSV-2: This type is more commonly associated with genital herpes, causing blisters and sores around the genital area. HSV-2 is almost exclusively transmitted through sexual contact.
Both types of HSV can cause similar symptoms, and it is often difficult to distinguish between them without proper medical diagnosis. It is important to note that having one type of HSV does not protect an individual from contracting the other type.
Early Signs of Genital Herpes
The first sign of infection you can resemble is a flu-like illness. This may occur within two days to three weeks after contracting the virus.
Symptoms of this flu-like onset can include:
- Headache
- Fever
- Fatigue
- Swollen lymph nodes
- Muscle pains
Additionally, some individuals may experience a tingling or itching sensation in the genital or anal area before the development of sores. It is essential to be aware of these early signs, as they can help in identifying the infection and seeking prompt medical attention.
Symptoms of Genital Herpes
The symptoms of genital herpes can vary from person to person, but may include:
It's important to note that the severity and duration of symptoms can vary from person to person, and some may experience no symptoms at all.
- Painful Sores or Blisters: Genital herpes is characterised by the development of painful sores or blisters that break and leave painful sores. This may take a week or more to heal completely.
- Burning Sensation when Urinating: Another common symptom is a burning sensation or pain while urinating, which can be quite uncomfortable.
- Unusual Discharge and Bleeding: Genital herpes can also cause smelly genital discharge and bleeding between menstrual periods, which should not be ignored.
- Additional Symptoms: Other symptoms may include headaches, fever, fatigue, muscle pains, and swollen lymph nodes, particularly in the groin area.
Many people with HSV are unaware of their infection, as they may experience no symptoms or only mild ones.
Symptoms typically appear 2 to 12 days after exposure and may include:
- Pain or itching in the genital area
- Small bumps or blisters near the genitals, anus, or mouth
- Painful ulcers that develop when blisters break and ooze or bleed
- Scabs forming as the ulcers heal
- Painful urination
- Urethral discharge
- Vaginal discharge
During the first outbreak, flu-like symptoms are common, such as:
- Fever
- Headache
- Body pain
- Swollen lymph nodes in the groin
Differences in Symptom Location
Sores develop at the site where the virus enters the body. The infection can spread if you touch a sore and then touch another part of your body, including your fingers or eyes.
The location of genital herpes lesions can vary depending on the individual and the type of HSV causing the infection. Lesions may occur in various areas, including:
- Vagina or vulva
- Penis
- Scrotum or testicles
- Buttocks or anus
- Thighs
- Buttocks
- Rectum
- Anus
- Mouth
- Urethra
- Cervix
It is important to note that HSV-1, which typically causes oral-facial herpes, can also cause genital herpes, particularly through oral sex. This means that lesions can appear on the genital area even if HSV-1 causes the infection.
Repeat outbreaks
After the initial outbreak of genital herpes, symptoms may return periodically, known as recurrent outbreaks.
The frequency of these outbreaks varies from person to person. They tend to occur more often in the first year after infection but usually become less frequent over time. Recurrent outbreaks are generally shorter in duration and milder than the first episode.
Some individuals experience warning signs, known as prodromal symptoms, a few hours or days before an outbreak. These may include:
- Genital pain
- Tingling or shooting pain in the legs, hips, or buttocks
Stages of Genital Herpes
Genital herpes typically progresses through several stages:
Primary Infection: This is the initial outbreak of genital herpes, which usually occurs within 2 to 12 days after contact with the virus. Symptoms may include:
Painful blisters or sores on the genitals, rectum, or mouth
Flu-like symptoms, such as fever, body aches, and swollen lymph nodes in the groin
Burning or tingling sensations in the affected area before the appearance of sores
Primary infection can last for 2 to 4 weeks
Latency: After the primary infection, the virus enters a dormant stage, remaining in the nerve cells. During this stage, there are no symptoms, but the virus can still be present in the body and can reactivate at any time.
Recurrent Episodes: When the virus reactivates, it causes recurring outbreaks, which are usually less severe and shorter in duration compared to the primary infection. Recurrent episodes may involve:
Mild tingling or itching sensations in the affected area before the appearance of sores
Fewer and smaller blisters or sores compared to the primary infection
Shorter healing time, typically lasting 3 to 7 days
These episodes can occur frequently, especially during the first year after infection. However, they tend to decrease in frequency and severity over time.
Causes of Genital Herpes
Genital herpes is caused by the herpes simplex virus (HSV), which spreads through direct skin-to-skin contact during sexual activity. There are two main types of HSV, both of which can cause genital herpes.
HSV-2
- HSV-2 is the primary cause of genital herpes. The virus can be present in:
- Blisters, ulcers, or fluid from ulcers
- The moist linings of the mouth, vagina, or rectum
- HSV-2 spreads through vaginal, anal, or oral sex, even when there are no visible symptoms.
HSV-1
- HSV-1 is commonly associated with cold sores but can also cause genital herpes. It is often acquired in childhood through close contact.
- A person with HSV-1 in the mouth can pass the virus to a partner’s genitals during oral sex.
- Genital herpes caused by HSV-1 tends to have fewer recurrent outbreaks than HSV-2.
- HSV does not survive well outside the body, making transmission through objects like towels or surfaces unlikely. However, kissing or sharing drinks may spread HSV-1.
Risk Factors
Several factors can increase your risk of contracting genital herpes:
Having multiple sexual partners significantly raises the likelihood of getting genital herpes. This may happen as each additional partner increases your exposure to the virus.
Engaging in direct sexual activities, such as oral, vaginal, and anal sex, can lead to the transmission of genital herpes.
People with weakened immune systems are more susceptible to genital herpes infections due to their compromised ability to fight off the virus.
Both herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2) can cause genital herpes. Although, HSV-2 is the primary cause of genital infections.
Understanding these risk factors can help you make informed decisions about your sexual health and take appropriate precautions. This helps to reduce your chances of contracting genital herpes.
Complications
If left untreated or managed improperly, genital herpes can lead to various complications:
- Neonatal infection is a serious concern, as the virus can be transmitted to an unborn baby before birth or during delivery. It can potentially cause life-threatening complications in newborns.
- Having genital herpes increases your vulnerability to other sexually transmitted infections (STIs), including HIV/AIDS. This is due to the presence of open sores and weakened immune defences.
- HSV infection can cause internal inflammatory disease, leading to swelling and inflammation within organs related to sexual activity and urination.
- The virus can spread to your fingers through breaks in the skin, resulting in a condition called herpetic whitlow. This condition causes discolouration, swelling, and painful sores on the affected finger.
- In rare cases, HSV infection can spread to the eyes, causing herpes keratitis. This may lead to pain, sores, blurred vision, and even blindness if not treated promptly.
Seeking timely medical attention and adhering to prescribed treatments can help minimise complications and manage the symptoms effectively.
Prevention of Genital Herpes
You can significantly lower your risk by adopting certain strategies:
Practice safe sex by consistently using barrier protection, such as condoms or dental dams, during sexual activity.
Maintain a long-term, monogamous relationship with a partner who has been tested for STIs and is not infected.
Avoid engaging in sexual contact when symptoms are present.
Discuss the risks with your partner and consider using antiviral medication to reduce the likelihood of transmission.
By being proactive and making informed decisions about your sexual health, you can minimise your risk of contracting genital herpes.
Diagnosis & Tests
Your healthcare provider can diagnose genital herpes based on a physical examination and your medical history.
To confirm the diagnosis, your provider may take a sample from an active sore for testing. Common diagnostic tests include:
- Viral culture: A sample from a sore is analyzed to detect the herpes simplex virus (HSV).
- Polymerase chain reaction (PCR) test: This test detects HSV DNA and identifies whether the infection is caused by HSV-1 or HSV-2.
- Blood test: In some cases, a blood test may be used to check for HSV antibodies and rule out other infections.
Your provider may also recommend testing for other sexually transmitted infections (STIs). If diagnosed, your partner should also get tested for genital herpes and other STIs.
Treatment & Management
There's no cure for genital herpes, but treatment can help manage symptoms and reduce outbreaks. Antiviral medications, self-care measures, and pain relief strategies are commonly used for:
- Reducing the severity and duration of outbreaks
- Helping sores heal faster
- Lowering the frequency of recurrent episodes
- Minimizing the risk of transmission to partners
Commonly prescribed antiviral medications include:
- Acyclovir
- Valacyclovir
- Famciclovir
Self-care measures such as keeping the affected area clean and dry, wearing loose clothing, and using cold compresses can help soothe irritation. Over-the-counter pain relievers like ibuprofen or paracetamol and topical lidocaine gels may provide additional relief. Your healthcare provider will determine the best treatment based on your symptoms and medical history.
When to See a Doctor?
If you experience symptoms such as blisters, sores, or pain in the genital area, it is important to consult a doctor. Seeking medical attention is particularly crucial if symptoms persist or worsen over time.
Pregnant women who experience a genital herpes outbreak should consult their doctor to discuss the risks and management of the condition. Specialised care may be necessary to minimise the risk of transmission to the baby during delivery.
Key Takeaways
Genital herpes is a chronic infection with no cure, but symptoms can be effectively managed.
Antiviral medications, such as acyclovir, valacyclovir, and famciclovir, are effective in reducing symptoms and preventing transmission.
Self-care measures, including keeping sores clean and dry, wearing loose cotton underwear, applying a cold compress, and taking Epsom salt baths, can help alleviate symptoms.
Pregnant women with genital herpes require specialised care to minimise risks to the baby during delivery.
Early diagnosis and treatment can help alleviate symptoms, reduce complications, and prevent infection to sexual partners.
FAQs
Is it possible to cure herpes completely?
Unfortunately, there is no cure for genital herpes. While symptoms may clear up independently, the blisters can recur. Treatment from a sexual health clinic can help manage outbreaks.
How serious is the herpes virus?
Genital herpes can be serious, especially for newborns. The virus may increase the risk of premature labour and transmission to the baby during pregnancy or delivery.
What impact can herpes have on my life?
Genital herpes can cause recurring outbreaks, pain, and discomfort. You must take precautions to avoid spreading the infection, but many people learn to manage their condition effectively.
Is it possible to transmit herpes to family members?
Yes, you can spread herpes to your family, particularly sexual partners. The virus can also be transmitted to an unborn baby during childbirth. Proper precautions can significantly reduce transmission risk.
How does genital herpes appear in the early stages?
The first stage of genital herpes involves small blisters that burst to leave open red sores around the genitals, anus, thighs, or bottom. Other symptoms include tingling, burning, or itching sensations.
What can I do to manage my genital herpes?
Visit a sexual health clinic for treatment. They can prescribe antiviral medicine to help manage outbreaks. Home remedies like ice packs, petroleum jelly, and keeping the genitals clean can ease symptoms.
Can genital herpes resolve on its own?
Genital herpes symptoms typically clear up on their own, but the blisters can recur. Treatment from a sexual health clinic can help manage the condition.
How can pregnant women protect their babies from genital herpes?
Pregnant women with genital herpes should consult their doctor for guidance on minimising transmission risks during pregnancy and delivery. Antiviral medication and a caesarean section may be recommended in some cases.
What conditions can mimic the symptoms of genital herpes?
Several conditions can mimic the symptoms of genital herpes, including syphilis, genital warts, molluscum contagiosum, and certain fungal or bacterial infections. A proper diagnosis from a healthcare professional is essential.
How do herpes simplex virus type 1 (HSV-1) and type 2 (HSV-2) differ?
HSV-1 primarily causes oral herpes (cold sores) and is typically transmitted through oral-to-oral contact. HSV-2 is the main cause of genital herpes and is usually spread through sexual contact.
References
American Academy of Dermatology. (n.d.). Genital herpes: Diagnosis and treatment. https://www.aad.org/public/diseases/a-z/genital-herpes-treatment
ASHA. (n.d.). Signs and symptoms of herpes—What you should know. https://www.ashasexualhealth.org/signs-symptoms/
Centres for Disease Control and Prevention. (2023, February 23). Genital herpes - CDC fact sheet. https://www.cdc.gov/std/herpes/stdfact-herpes.htm
Minnesota Department of Health. (2022). Genital herpes. https://www.health.state.mn.us/diseases/herpes/genitalherpes.html
NHS inform. (2022, December 2). Genital herpes. https://www.nhsinform.scot/illnesses-and-conditions/sexual-and-reproductive/genital-herpes/
Yale Medicine. (n.d.). Genital herpes. https://www.yalemedicine.org/conditions/genital-herpes
Check Related Salts
Browse Other Conditions
Latest health articles
Top Health Essentials
Disclaimer
Top-Selling Medicines:
Top-OTC medicines:
...View more
Company
About UsHealth ArticleHealth StoriesDiseases & Health ConditionsAll MedicinesAll BrandsNeed HelpFAQSubscribe
Registered Office Address
Grievance Officer
Download Truemeds

Contact Us
Our customer representative team is available 7 days a week from 9 am - 9 pm.
v3.7.10
Our Payment Partners